ACT Public Hospitals Hit by Predicted Health Tsunami

Following the release of the latest report of the Australian Institute of Health and Welfare (AIHW)[i] that showed the ACT’s hospital performance dipping to yet another record low, the Minister for Health Ms Rachel Stephen-Smith is reported to have sought to explain away the poor outcome by claiming that “Canberra’s hospitals had seen not only increased presentations, but more complex patients”[ii].
Further decline in performance was reported just a week later following the release of the quarterly health report[iii]. Across the Territory’s hospitals, just one in four patients in the urgent category were treated within the clinically recommended time. In the Canberra Hospital, the principal tertiary hospital, only one in five patients in this category received treatment within the clinically recommended time. The national rate is almost three times higher. Most worryingly, the target of 100% for category 1 patients, where resuscitation is required, was not met.
The persistent and increasingly poor performance of our hospitals begs the question: “How and why did the hospital system in the nation’s capital, the jurisdiction with the highest average incomes in Australia, reach such a parlous state?” Minister Stephen-Smith again proffered the explanation of unprecedented demand and more complex patients[iv].
The assertion about “increasing complexity” was strongly challenged by the Australian Medical Association ACT President Dr Antonio Di Dio who said the Minister should produce evidence that showed ACT patients were more complex than other jurisdictions, if she was to claim that as a reason for the figures. He is also reported to have said that it came down to inadequate resourcing, in terms of both beds and staff, throughout Canberra Hospital[v].
Before addressing the claim of unprecedented demand and increasing complexity it would be useful to make some observations about the level and composition of emergency department presentations in the ACT. A comparison of emergency department presentations between the September and June quarters indicates that Category 1 to 3 presentations constituted a relatively larger proportion of the total presentations in the September quarter. This is in large part due to the number of presentations in Category 4 and 5 decreasing in the September quarter, and the total presentations also decreasing slightly. The decrease in the number of less urgent patients may be due to the transfer of that demand to the walk-in centers, or to General Practitioners, consistent with the Government’s policy objectives and its advice to Canberrans. Table 1, below, provides a direct comparison by category, of all presentations for the two quarters.
Table1: Emergency Department Presentations and Treatment Times by Triage Category
Source: ACT Government
The comparison reveals that there is absolutely no evidence to support the Minister’s claim of increasing complexity. Indeed, high level comparisons of relative stay and average cost weight indicate that, as a whole, the ACT’s hospital system does not experience any higher level of complexity than the States. In any event it is hardly a valid excuse for failing to treat patients, in the urgent and emergency categories, on time.
We agree with Dr Di Dio’s assessment that the suggested “increase in complexity” is merely a distraction, and ultimately, the declining performance is due to inadequate staffing and beds. Indeed, we have previously pointed out that since 2012-13, Canberra’s health system has endured funding cuts of approximately 1% per annum in real terms, when taking into account actual population growth, ageing, changes in technology, and inflation in prices of medicines and wages[vi], and that the system’s capacity to deliver safe services has been severely eroded[vii].
It is moot then to also ask: “Is the Territory’s health system, as repeatedly claimed by the ACT Government, suffering from unprecedented population growth?” Table 2 below provides a comparison of the annual growth rate during the period 2011-12 to 2017-18 with that over the previous four years. Whether considered on a year-on-year basis, or on a through-the-year average basis, data from the ABS reveals that population growth rate in the ACT over the last six years has, in fact, been relatively lower than it was in the previous four years.
Table 2: Population Growth Rate
Source: Australian Bureau of Statistics
Accepting that there is no evidence to support either of the Ministers explanations for the poor performance of our public hospitals could there be factors, other than population growth, for the unprecedented demand claimed by the Minister? We accept that barring any seasonal or unusual fluctuations, and in the absence of major policy shifts, demand will increase every year and as such it might be claimed to be unprecedented compared to an earlier time. The pertinent question is, however, whether the recent growth in demand had been unanticipated and was not predicted.
If the answer to that question is “yes” then the Government should explain why it had failed to predict or plan for meeting such a fundamental need as a fully functioning and safe public health system.
However, the answer to the question is, of course, unequivocally “no”.
The current levels of demand for hospital services in the ACT and its rate of growth were both anticipated and planned for as early as 2008. The then Minister for Health, Ms Katy Gallagher had not only developed, with the full support of the then Cabinet and Government, a detailed plan to meet the Territories future health needs but she had also secured an initial $300 million through the budget process to implement a $1 billion program of investment in hospital and health infrastructure.
In a media release on 15 June 2008, then Minister Gallagher said[viii]:
“Detailed modelling work by ACT Health has confirmed that with one of the fastest ageing populations in the country, the ACT community is facing a ‘health tsunami’ in the next decade, unless detailed and brave investment is made now.”
Ms Gallagher also announced that:
“[T]he 2008-09 budget included a $300 million investment in health infrastructure, including a Womens and Childrens Hospital and a new suite of mental health facilities”. She further noted that this was only the first stage of the plan for meeting the future needs of the community and the Government would be consulting with GPs in the coming months and years around further large investment in our health facilities."
A discussion paper titled “Expanding hospital services in the ACT: an additional 400 Hospital Beds” was released by Ms Gallagher in February 2011 to seek community input on the delivery of an additional 400 hospital beds[ix]. It included the following statement:
“The existing ACT public health care system is at capacity and needs to expand to meet future health demand created by an ageing and growing population, changing technology and consumer expectations.
Recent investments by the ACT Government to enhance the capacity of community health centres and the introduction of the nurse led Walk-in-Centre, are focused on reducing demand on public hospital services. Notwithstanding these initiatives, the pressure on acute beds will continue with projections estimating a 50 per cent increase in admissions up to 2022.”
The ACT Government was well aware, over a decade ago, of the increase in demand, was also cognizant of the capacity limitations of the health system at that time to meet future demand pressures and so committed to increasing its capacity through a program of investments. The foreshadowed increase in beds was part of a $1 billion Capital Asset Development Plan (CADP) developed by Ms Gallagher and fully supported by the then Government, including through the budget.
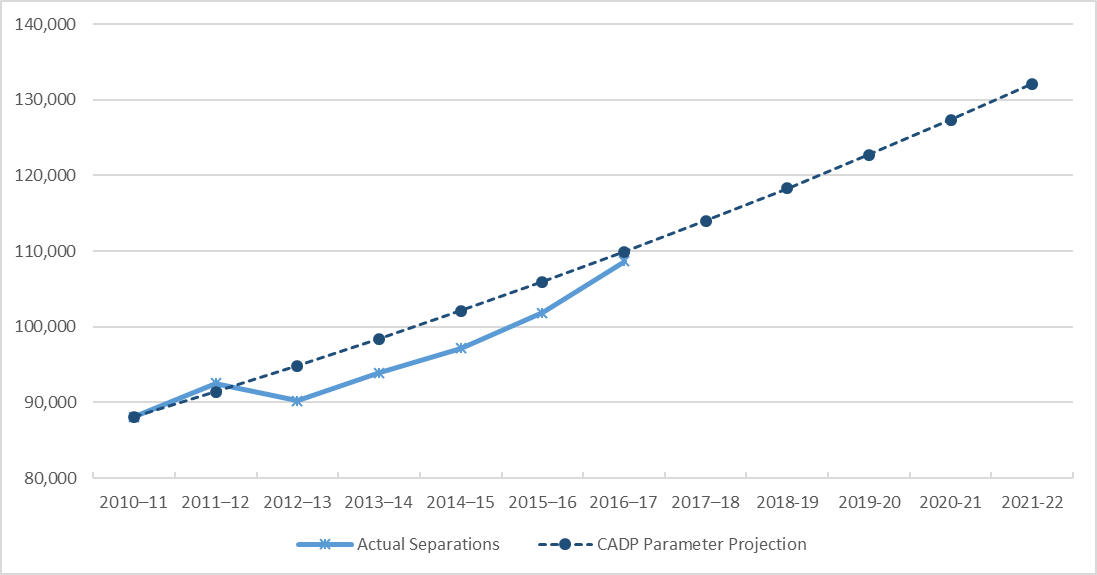
It is instructive, a decade on from its development, to assess how current actual demand and bed supply compare with the CADP projections? Chart 1 below shows the actual number of admissions in the ACT hospital system (solid line) as reported by the Australian Institute of Health and Welfare compared with the projections based on CADP growth assumptions (dashed line).
Chart 1: Acute Patient Separations - ACT Public Hospital System and CADP Planning Assumptions
Source: Australian Institute of Health and Welfare.
It is clear from the data that the actual activity level as measured by acute patient separations remained below the projections based on CADP assumptions during the period 2012-13 to 2016-17 (the last year for which the AIHW data is available). Based on the activity increasing by 50% to 2022, the annual growth assumption under CADP was an average of 3.75%. It is also the case that activity growth over the years 2014-15 to 2016-17 had averaged 5% reaching close to the CAPD planning projection level. In light of this one would have expected the Government to at least have continued to implement the remaining part of the program of investments designed by then Health Minister, Katy Gallagher. Unfortunately, the opposite occurred.
Chart 2, below, shows the CADP bed demand projections (dashed line), adjusted projections to achieve optimum bed occupancy of 85%, and actual bed availability. Notably, up to 2015-16, the trajectory of bed supply matched the bed demand projection, albeit, at a slightly lower level. During this period, the first tranche of CADP initiatives appear to have been effective in reducing demand and delivering additional beds.
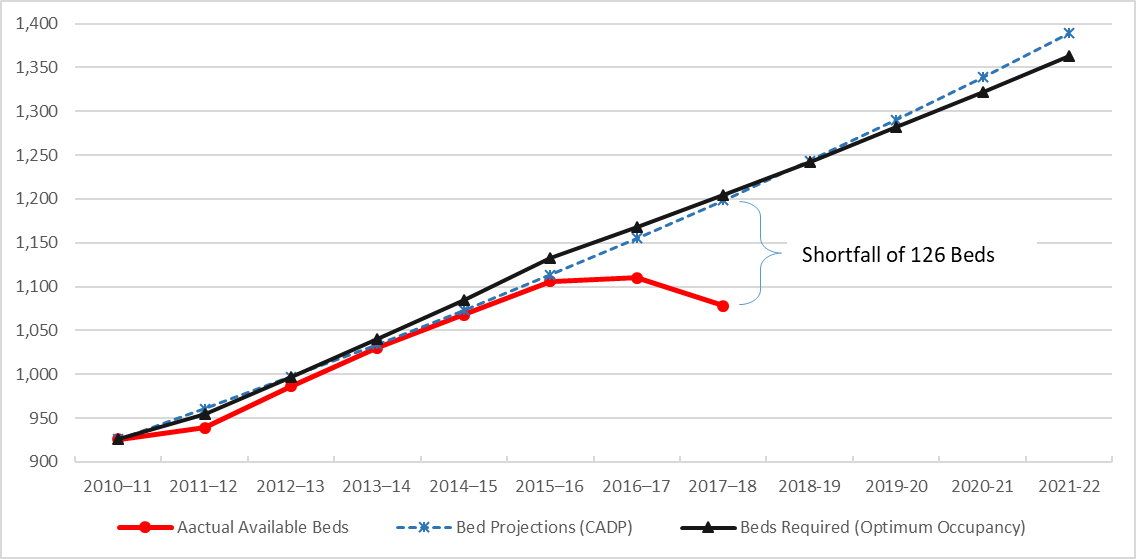
It is clear, however, that significant decisions were taken in 2015, following Katy Gallagher’s resignation as Chief Minister and her move to the Senate, which resulted in a sudden and dramatic reduction in the number of available hospital beds. Not only was the plan to deliver the additional 400 beds abandoned, but the withdrawal of funding in real terms forced bed closures, which resulted in the bed occupancy rate at the Canberra Hospital spiking to 94% or 9% higher than the bed occupancy target of 85%. We estimate that the resultant shortfall in 2017-18 between the beds required and beds supplied in Canberra public hospitals was 126 beds.
The first tranche of the $300 million allocated for CADP provided for a suite of investments to reduce demand on the acute health care system as well as increasing its capacity including a Women’s and Children’s Hospital; mental health facilities; refurbishment and construction of Community Health Centres; improved breast cancer screening facilities; and Neurosurgery Suite with the latest in imaging systems.
The Budget also committed to $63.8 million for feasibility and forward design works[x] for a number of projects in the second tranche including the full redevelopment of the Canberra Hospital site[xi]. The redevelopment plan was based on a master plan for the site developed[xii] through extensive consultation with a broad range of stakeholders[xiii].
Those projects, including the master plan for the site were, however, also abandoned by the current Government. It decided instead to proceed with a significantly watered-down proposal known as the Surgical Procedures, Interventional Radiology and Emergency Centre (SPIRE) for the Canberra Hospital. This project has already been deferred twice and is now foreshadowed to be completed in 2024. It is planned to deliver only 148 beds[xiv], approximately one third of the number originally planned, and almost a decade late, by which time it is estimated an additional 400 beds will be required over the 2017-18 bed numbers based on the current growth estimates.
In short, if SPIRE was operational today it would be fully utilized and a further two similarly sized hospital bed supply projects would still need to be delivered by 2024 in order to meet currently estimated growth in demand for hospital beds.
A shortage of hospital beds of the order that currently exists in Canberra obviously has potentially serious consequences for every resident of Canberra. As with all policy choices or funding decisions made by Government it is important to understand their broader distributional impact. It would be illuminating to see any analysis the Government has of the distributional effect of its health policy.
[i] Australian Institute of Health and Welfare (December 2019); Emergency Department Care, at https://www.aihw.gov.au/reports-data/myhospitals/sectors/emergency-department-care.
[ii] The Canberra Times (11 December 2019), ACT emergency department wait times blow out, at https://www.canberratimes.com.au/story/6535818/act-emergency-department-wait-times-blow-out/.
[iii] ACT Government (2019); ACT Public Health Services Quarterly Performance Report: July to September 2019, at https://www.health.act.gov.au/sites/default/files/2019-12/QPR Q1 19-20.pdf.
[iv] The Canberra Times (18 December 2019), Hospital ED performance hits record low again, at https://www.canberratimes.com.au/story/6549295/canberra-hospitals-ed-performance-hits-record-low-again/?cs=14229.
[v] The Canberra Times (12 December 2019), ACT health performance a disgrace, https://www.canberratimes.com.au/story/6538389/acts-health-performance-a-disgrace/.
[vi] The Canberra Times (30 March 2019); The ACT government is shrinking health spending year on year, at https://www.canberratimes.com.au/national/act/the-act-government-is-shrinking-health-spending-year-on-year-20190319-p515fd.html.
[vii] Institute for Governance and Policy Analysis (2019), Signs of an Unsafe ACT Hospital System for Patients as well as Practitioners, at /2019/10/293-signs-of-an-unsafe-act-hospital-system-for-patients-as-well-as-practitioners.
[viii] Media Release (15 June 2008), at http://info.cmtedd.act.gov.au/archived-media-releases/media05eb.html?v=6913&s=195
[ix] ACT Government (2011); ACT Public Hospital Services: Delivery of Additional Hospital Beds - Options Analysis, at https://www.parliament.act.gov.au/__data/assets/pdf_file/0015/373011/06._ACT_Government_-_Options_Analysis.pdf.
[x] ACT Government (2008); Budget Paper No. 1, 2008-09 Budget, at http://www.treasury.act.gov.au/budget/budget_2008/files/paper1/bpaper1.pdf.
[xi] ACT Government; Your Health – Our Priority: Ready for the Future, available in the ACT Heritage Library for viewing only.
[xii] ibid.
[xiii] Health Care Consumers Association Inc. (2016); Consumer involvement in health infrastructure in the ACT, 2009-2016, at https://www.hcca.org.au/wp-content/uploads/2018/04/Consumer-involvement-in-health-infrastructure-projects-in-the-ACT-2009-2016-FINAL-DECEMBER-2016.compressed.pdf.
[xiv] ACT Government (2019); Features of SPIRE at Canberra Hospital, at https://health.act.gov.au/sites/default/files/2019-05/SPIRE Factsheet_2019_Release 2.pdf.


.png)
.png)